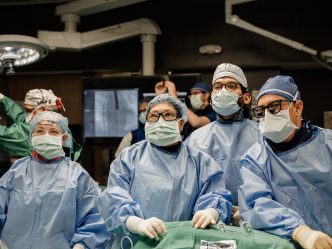
More than half of rural hospital patients are now admitted through emergency departments, said Catherine Clary, director of the Center for Rural Health Support and Study at Augusta University Medical Center.
“The emergency department has become the hospital’s front door. When we look at the data, we see that nearly all of the growth in hospital admissions since the early 1990s can be attributed to an increase in emergency department visits.”
The Centers for Disease Control and Prevention estimated that emergency room visits resulted in 12.2 million hospital admissions in 2013, and according to Clary, much of that volume can be seen in rural hospitals, where the emergency room is often the sole primary care provider for the community.
“Greater emergency department volumes in rural hospitals often reflect a shortage of primary care services and larger numbers of uninsured patients,” she said. “Because emergency departments are bound by law to provide care, often without compensation, uninsured patients are turning to the local hospital emergency department more and more often.
Clary said emergency services in Georgia’s rural hospitals was a primary area of focus for a task force Augusta University President Brooks Keel stood up in 2015 in response to the closure of more than eight of Georgia’s rural hospitals since 2001.
“One of the committee’s recommendations was that rural hospitals should serve as the entry point for emergent care. In other words, they are the gateway to specialized facilities and are instrumental in diagnosing and stabilizing patients before transfer.”
Because the aim is to have patients in rural communities consider their local emergency room as their first choice for emergent care, Clary said the community must have confidence in the medical staff and the level of care they’ll receive.
“One of the biggest challenges for rural hospitals is physician recruitment,” she said. “Many physicians prefer to work in urban areas, where there are more career and professional development opportunities. There’s also family and lifestyle considerations to take into account.”
Clary said Augusta University Medical Center and Washington County Regional Medical Center, located in Sandersville, Georgia, are working together to overcome these challenges. The two hospitals entered into an agreement this month, where AUMC – the state’s leader in specialty and subspecialty care – will provide the Sandersville hospital inpatient and emergency services.
Dr. Michael Hocker, vice chairman of the Department of Emergency Medicine and the J. Harold Harrison, MD, Distinguished Chair in Emergency Medicine at Augusta University’s Medical College of Georgia, said that while the emergency services agreement was officially inked this month, the university began providing hospitalist coverage for Washington County Regional Medical Center last fall, and some specialties and services have been present at the hospital even longer.
“Our job is to provide these hospitals with the tools they need to be successful,” he said. “We want to provide Sandersville residents access to the best acute and emergent care, but we need to be able to do that where they live. We want them to consider their local hospital as not just the only option, but also the preferred option.”
In addition to personnel, Augusta University Medical Center will use telemedicine technologies to provide patients remote access to physicians in Augusta, Hocker said.
“Our telemedicine network extends to emergency departments across the state. Oftentimes, we’re able to provide diagnosis and treatment without the patient ever having to leave their local hospital. This can be lifesaving when we talk about diseases such as stroke, where seconds count.”
Hocker said he hopes patients in Sandersville who may be receiving care elsewhere return to their local hospital.
“We want people to know we’re invested in the community,” he said. “We’re providing advanced education and training for hospital staff and will have residents and other health professions students begin rotations at the hospital. This ensures a future generation of providers equipped to better care for our rural communities.”
 Augusta University
Augusta University