Being prepared and having a game plan are paramount in the medical field. For those working in Rehabilitation Services at Augusta University Medical Center, getting the information and sharing it has made the past two months battling COVID-19 a little bit easier.
Dan Fisher, Rehab Therapy Services Inpatient Rehab team leader, says information is being shared from around the world on treatment and management of COVID-19 patients, allowing AUMC to better prepare for what was coming. Rehab staff have been attending webinars, reading professional literature and searching the internet for information, then sharing it with the team to develop the best course of action for their role in the treatment of local COVID-19 patients.
“When the hospital stopped outpatient procedures and outpatient clinics closed down for a period of time, we started working with our outpatient counterparts to train and orient them in our area,” Fisher said. “That was a big team effort. We were anticipating that our volume would increase or our staff would get sick, or both. We didn’t want to be short on staff, so we were planning for reserve providers from outpatient areas.”
Senior occupational therapist Wendy Jones said everyone works together as a cohesive team and communicates well across all of their professions. But now with different obstacles in their way, she feels they are all stepping up to the challenge and learning from each other’s experiences.
Jones is a veteran at the hospital and said she doesn’t have any sort of reference to fall back on, because nothing like this has happened during her tenure.
“When we’re trying to problem solve, we’re definitely giving each other a hand when we need to,” said Jones, who has worked at AUMC for more than 20 years. “We’re trying to limit how many people are exposed from our department. We’re comparing notes and trying to see if there’s an effective rehab treatment to help a particular person. I think just sitting down and sharing what things we’re seeing that aren’t typical of our regular caseload has been helpful … It’s a learning process.”
Physical therapist Caroline Shore has been out of school just under three years. She had been working in the ICU before the pandemic and said seeing the differences in typical ICU care for these patients has been eye-opening. She agrees with Jones that everyone works great as a team and communication is at an all-time high right now.
“I personally really like (the communication). I hope this is something that sticks around and becomes part of our culture,” Shore said.
Speech pathologist Kathleen McHugh said she is thankful co-workers are looking out for one another. She said one of her greatest challenges is getting the patients to hear her while she’s in the room with all of the machines running and trying to talk through a mask.
“It’s important that people can hear me; it’s really hard for your patients to hear you and understand what you’re saying,” McHugh said. “Wendy has helped me a lot … Or trying to write something down on a paper towel in the room and seeing if the patient can read that back to us. The challenges are something I haven’t really seen as much as what we’re seeing right now with these patients.”
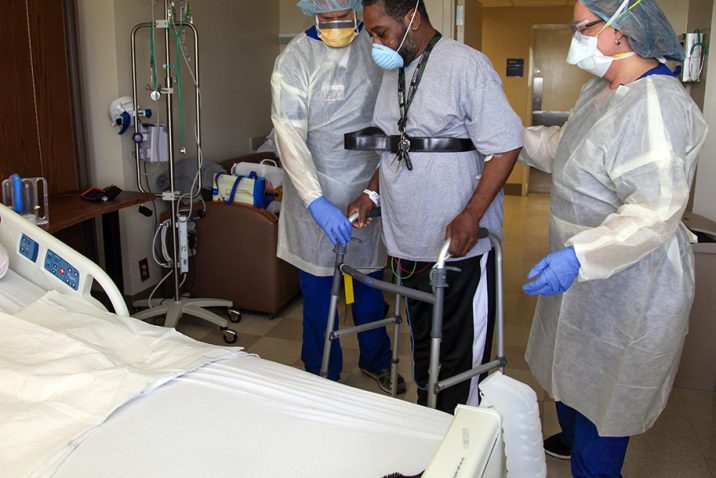
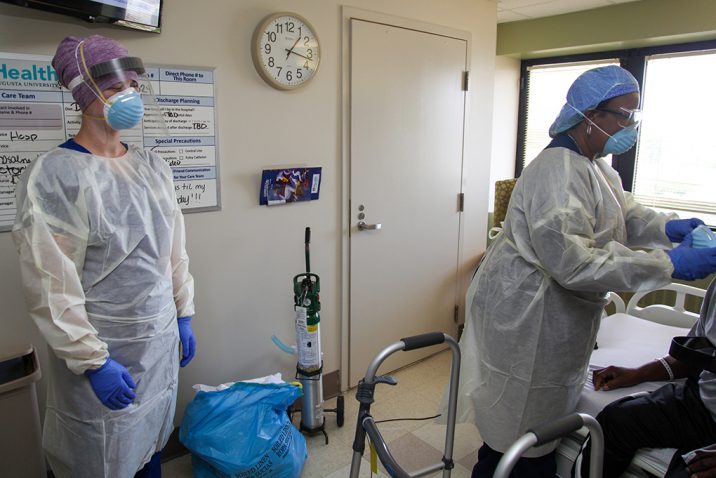
Senior physical therapist Marc Brody said one of his biggest adjustments to daily operations is wearing the PPE for extended periods of time. Staff working with COVID-19 patients in the ICU setting wear a gown, N-95 mask with a surgical mask over the top and a a face shield or goggles. He also notes staff need to make sure they have everything needed before entering the room to conserve PPE.
“I’ve been learning to slow things down and be patient and take my time … You try to anticipate every need you have prior to entering the patient’s room,” Brody said. He notes there is a lot of equipment and lines, making it difficult to maneuver in a tight space. “It’s physically and mentally a little more exhausting than a typical day but there is an overwhelming sense of satisfaction and accomplishment. It’s a new challenge and it’s exciting.”
Jones said they have been trying to do as much as they can each time they enter a COVID-19 patient’s room. The therapists are communicating with other staff outside of the room to handle as many tasks as possible while they are in the room, reducing staff exposure and PPE use.
All agree getting to see patients like Caroline Maddox be able to leave the hospital after battling the COVID-19 virus has been satisfying.
“We all got to watch Ms. Maddox get in a wheelchair and wave as she was leaving the floor and we had all been working with her since she got out of the ICU and went to the regular floor,” Jones said. “And to see her go from being unable to even sit up on the side of the bed to get up and get into a wheelchair and leave to go home to her family was a very satisfying … It was a very good day for us.”
“The hardest part is patients are not allowed any visitors,” Brody said. “Some of the patients or their families aren’t from this area, so we’re kind of there for them as a friend and confidant and trying to get through this experience with them.”
Fisher said he hasn’t seen anyone who has needed to be “nudged,” with everyone jumping in when needed.
“I’ve been extremely impressed with how self-motivating and direct the staff have been, and just seeing the need and going and taking care of it,” he said. “These four are the ones who jumped right in and led the way into figuring out what our role in taking care of these patients was going to be.”
 Augusta University
Augusta University