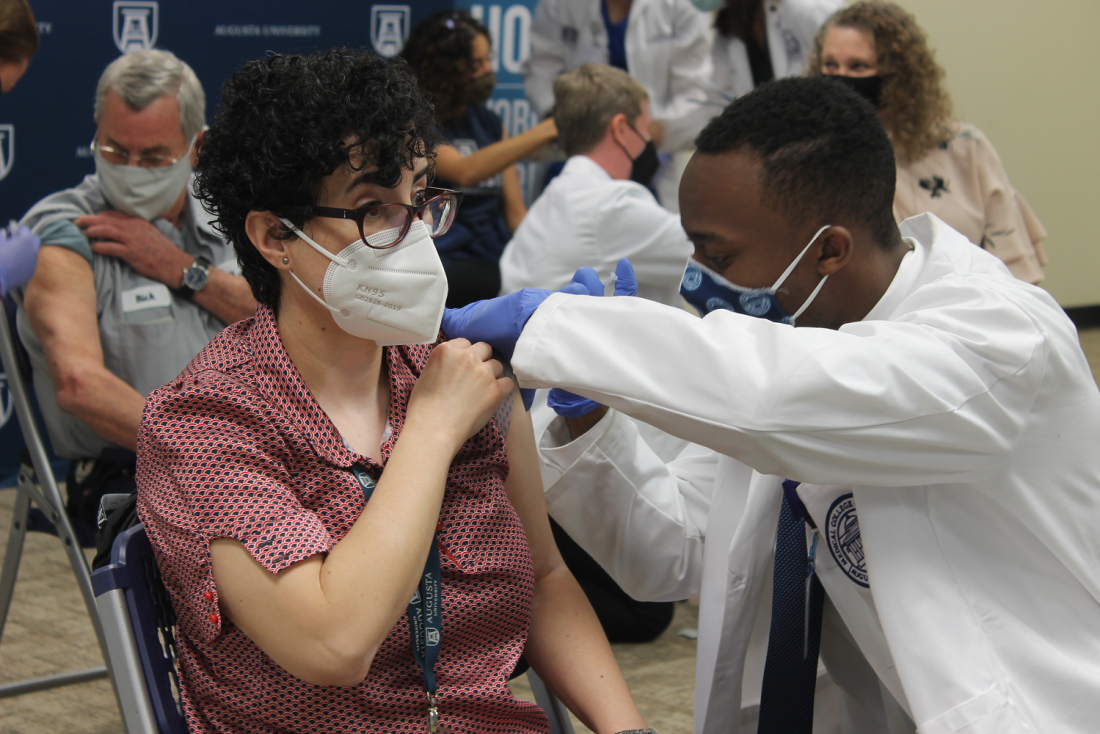
Misconceptions and misinformation about the COVID-19 vaccines continue to circulate, especially amid updated federal vaccine guidance. Myths like this might seem harmless, but they can generate enough uncertainty to breed vaccine distrust, which helps vaccine-preventable diseases persist.
MYTH 1: The mRNA technology used to make the COVID-19 vaccines is brand new.
The Pfizer-BioNTech and Moderna COVID-19 vaccines are synthetic mRNA (messenger RNA) vaccines, which means they contain biochemical instructions for making protein antibodies. They are the first mRNA vaccines to be tested in large-scale phase III human trials, but mRNA vaccine technology is not new.
Researchers have been working with mRNA vaccines for decades for influenza, Zika, rabies and cytomegalovirus.
MYTH 2: The vaccine must be ineffective, since we’re offering booster shots.
Booster shots do not indicate an ineffective vaccine. Booster shots are routine for multiple vaccines, including those for tetanus, diphtheria and pertussis (whooping cough).
A booster just means that over time, immunity from a disease naturally begins to wane. As of Oct. 27, only those at high risk of severe COVID-19 (including health care personnel, the immunocompromised and those over age 65) should receive boosters.
MYTH 3: The vaccine has a microchip in it.
This is false and is serious disinformation. Reuters and other media outlets have debunked this multiple times. The syringe used to administer COVID-19 (typically a 22 gauge needle) is too small to contain a microchip that’s capable of tracking someone’s location.
MYTH 4: Since COVID-19, like the flu, is caused by a virus, I don’t need my flu shot if I’m vaccinated.
This is false. Many health experts argue that getting the flu vaccine this year is more important than ever, as a “twindemic” of both COVID-19 and the flu can overwhelm local hospitals.
The 2020-21 flu season resulted in the fewest flu cases ever recorded, likely because methods that prevent COVID-19 (wearing masks, social distancing, regular handwashing etc.) are also effective at preventing the flu.
But now that lockdown restrictions have lifted in most states and people are interacting more, experts predict this year’s flu season will be worse than last year. You can receive the flu vaccine and the COVID vaccine at the same time.
MYTH 5: Not getting vaccinated only affects me.
The COVID-19 pandemic is a public health issue, and therefore fighting it, experts argue, requires cooperative public effort.
During the most recent case surge in September, hospitals in the CSRA were so overwhelmed with unvaccinated COVID-19 patients that the care of others — including their surgeries, checkups and biopsies — was put on hold.
MYTH 6: I shouldn’t bother getting vaccinated because I still might get COVID-19 anyway.
While no vaccine is 100% effective at preventing infection, the COVID-19 vaccine works exceedingly well at preventing severe symptoms from the virus.
Among the fully vaccinated who still get infected with COVID-19, their symptoms are almost always less severe, meaning they are much less likely to be hospitalized or die than unvaccinated people.
Experts reassure that “breakthrough infections” do not indicate COVID-19 vaccines are failing. Since vaccinations became available, AU Health statistics show the majority of patients hospitalized for COVID-19 are unvaccinated.
MYTH 7: The vaccine must not be safe, since reports are growing of serious side effects post-vaccine.
Although adverse effects have been reported, side effects are a possibility for all vaccinations and medical procedures. This does not mean the risks outweigh the benefits. This also does not mean that all “adverse events” reported are in any way caused by vaccination.
As of Nov. 4, over 425 million doses of COVID-19 vaccine have been administered in the U.S. under the most intense safety monitoring in national history — a strong indicator of their safety. However, everyone should discuss their concerns with their primary care provider.
MYTH 8: The vaccine is dangerous for pregnant people.
Hundreds of thousands of people have received a COVID-19 vaccination during pregnancy and no safety concerns have been reported.
Additionally, the Society for Maternal-Fetal Medicine, the American College of Obstetricians and Gynecologists and other obstetrics experts recommend vaccination for pregnant people. These endorsements were made due to the well-cited dangers of contracting COVID-19 during pregnancy.
An April 22 study from JAMA Pediatrics, a peer-reviewed journal published by the American Medical Association, found that pregnant women who contract COVID-19 are at higher risk for preeclampsia/eclampsia, severe infections, intensive care unit admission, maternal mortality, preterm birth and more.
Regardless of whether pregnant people choose vaccination, they should take strong precautions to avoid contracting COVID-19 in the first place, and should discuss vaccination with their obstetrician.
Review the Augusta University COVID-19 resources. Employees and the community can schedule a vaccination through AU Health. Read the U.S. surgeon general’s advisory on confronting health misinformation.
 Augusta University
Augusta University