AUGUSTA, Ga. – A cutting-edge procedure at Georgia Regents Medical Center is helping terminal liver cancer patients live longer.


“For people who are out of other options, including chemotherapy and surgery, transarterial radioembolization can offer hope by adding as much as three to four years to their lives,” said Dr. Eran Rotem, the interventional radiologist who brings this minimally invasive procedure to patients who otherwise might have just months to live.
“This means more time to walk a daughter down the aisle or see a grandchild born. Added time to life is priceless, and we want people facing this diagnosis to know that there may be another treatment method for them, even though it is not yet widely known and used,” Rotem said.
Until recently, patients would have to drive to Atlanta or travel even farther distances to large cancer centers like M.D. Anderson in Texas or Memorial Sloan Kettering in New York for transarterial radioembolization, an image-guided approach in which Rotem delivers an extremely high dose of radiation via tiny glass beads directly to the cancerous tissue inside the liver, effectively killing the malignant cells.
In order to target the tumor and minimize risk to healthy tissue, a pre-treatment mapping procedure is required about a week before the actual treatment.
“During this trial run, we inject a safe dose of nuclear medicine tracer into the patient’s vessels so that we can track the blood flow and block off, or embolize, the paths leading out of the liver. That way when we treat with the yttrium isotope – the radioactive Y-90 spheres – we are able to contain the radiation in the targeted area only. This will ensure that the Y-90 doesn’t escape to surrounding tissues and organs,” Rotem said.
The pre-treatment mapping also enables the radiologist to tailor the treatment to the location and size of the tumors in each patient’s liver.
Then, using a nonsurgical, image-guided intervention, Rotem inserts a catheter through a tiny cut in the patient’s groin and snakes it through the arteries until it reaches the hepatic artery, or main artery to the liver. Next, he discharges millions of tiny radioactive beads through the catheter that become trapped inside the smaller vessels feeding the tumor, essentially blocking the supply of blood to the cancer cells while also emitting a high dose of radiation to the tumor.
The Y-90 beads will continue to release radiation over the course of several weeks following treatment, gradually decreasing to insignificant levels and with few side effects.
Y-90 radioembolization is used to treat tumors that began in the liver or have spread, or metastasized, to the liver from another part of the body. It is a palliative treatment, which means it does not provide a cure but instead helps slow down the growth of the disease and alleviate symptoms. The procedure is an option for patients who are not candidates for other treatments, including surgery or liver transplant.
The whole liver can usually be treated in one session with Y-90. However, in some cases the right and left lobes of the liver may need to be treated separately with one month between each treatment.
Because it is less invasive, hospitalization is rarely needed, and the entire procedure is usually finished in about an hour. Studies show it is well-tolerated by patients, and the treatment is so specifically targeted, that there is little impact to surrounding healthy tissues.
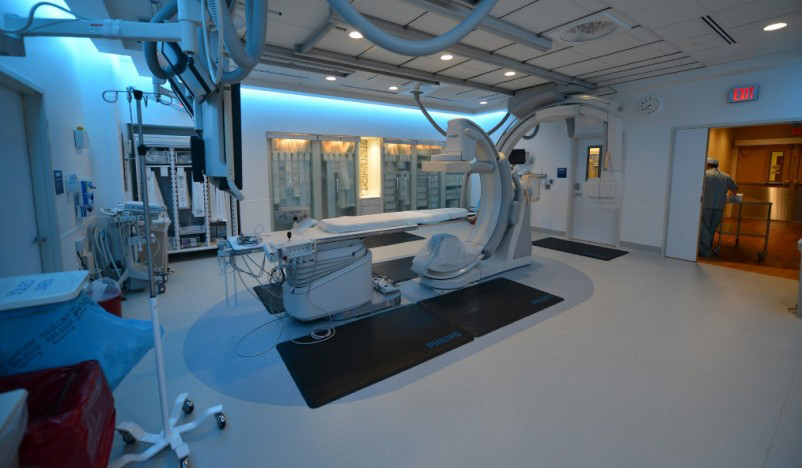
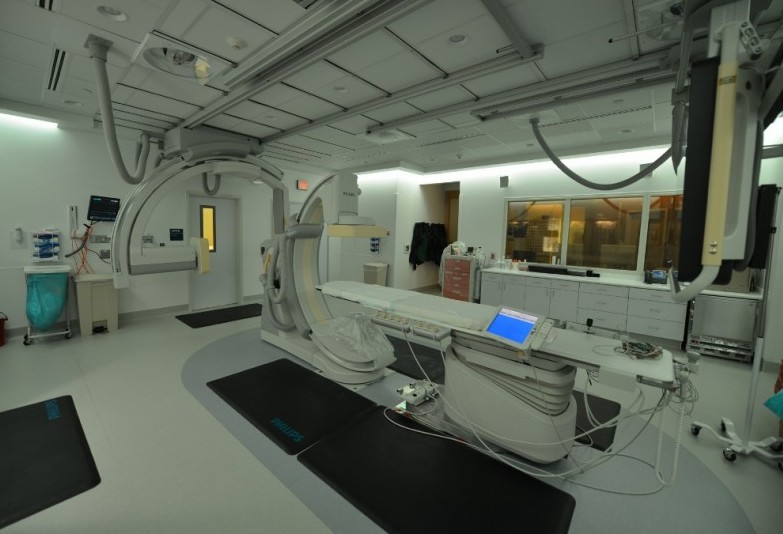
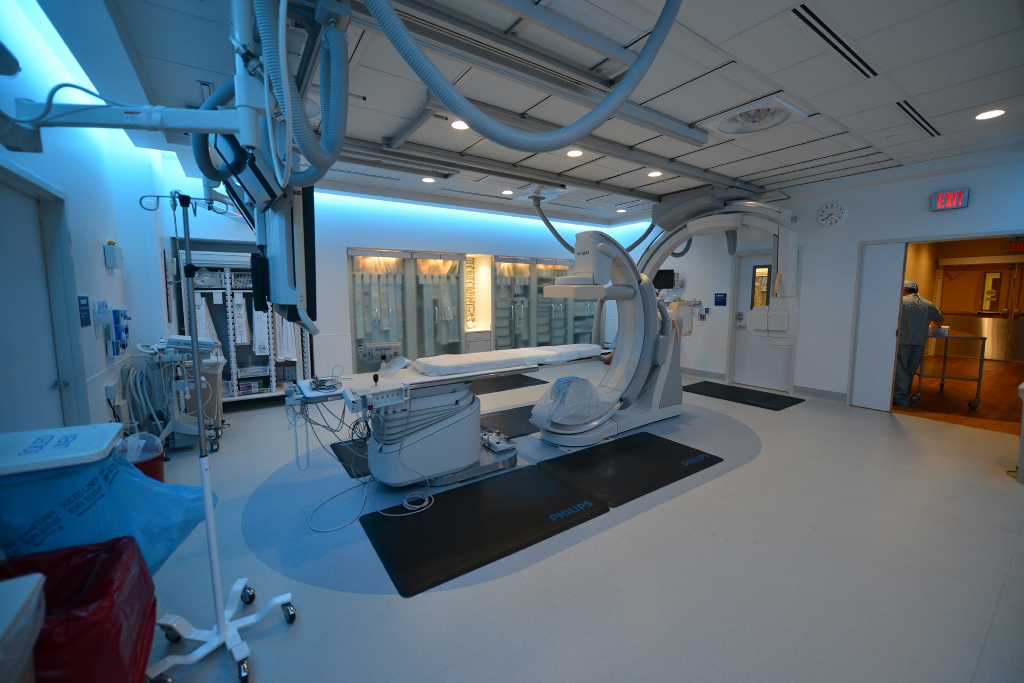
Mapping and treatment are both outpatient procedures performed in the hospital’s state-of-the-art interventional radiology suite, also called the Philips Allura FD Biplane room. The Philips XperCT is used for mapping, and fluoroscopy imaging allows Rotem, the Chief of Vascular and Interventional Radiology, to visualize the actual Y-90 radioembolization.
The suite was designed exclusively for interventional radiology at Georgia Regents Medical Center with input from physicians, imaging specialists, patients, families and in-house experts from Philips Healthcare as one of many projects in the 15-year, $300 million alliance the two organizations signed in June 2013.
Through this first-of-its-kind alliance, GRHealth and Philips are working to develop a new model for the health care industry that stresses better outcomes for patients through innovation, new technologies and collaboration. More than a dozen health care strategists, trainers and technology experts with Philips work directly with the GRHealth team on a daily basis, operating out of the new Philips Learning Center on the top floor of the medical center.
Media Inquiries:
Denise Parrish
Senior Media Relations Coordinator
706-721-9566 Office
706-831-3148 Cell
mparrish@gru.edu
 Augusta University
Augusta University